Treatments And Causes Of Achilles Tendonitis
Overview
 Achilles Tendinitis is a common overuse injury which results in inflammation of the achilles tendon, most frequently causing mild to severe heel pain. The achilles tendon is the largest tendon in the body, connecting your calf muscle to your heel bone. It?s used with every step - when you walk, run, and jump. Although the Achilles tendon can withstand great stresses, it?s also prone to tendinitis. The condition is very common in athletes, especially runners who?ve suddenly increased the intensity or duration of their workouts. It?s also common in middle-aged, ?weekend athletes? who play sports like tennis or basketball only occasionally. The pain from achilles tendinitis may be felt anywhere from the back of the leg to the top of the heel. Most cases are mild and can be treated at home under a podiatrist?s supervision. Severe cases of Achilles tendinitis can lead to tendon tears (ruptures) that may require surgical repair.
Achilles Tendinitis is a common overuse injury which results in inflammation of the achilles tendon, most frequently causing mild to severe heel pain. The achilles tendon is the largest tendon in the body, connecting your calf muscle to your heel bone. It?s used with every step - when you walk, run, and jump. Although the Achilles tendon can withstand great stresses, it?s also prone to tendinitis. The condition is very common in athletes, especially runners who?ve suddenly increased the intensity or duration of their workouts. It?s also common in middle-aged, ?weekend athletes? who play sports like tennis or basketball only occasionally. The pain from achilles tendinitis may be felt anywhere from the back of the leg to the top of the heel. Most cases are mild and can be treated at home under a podiatrist?s supervision. Severe cases of Achilles tendinitis can lead to tendon tears (ruptures) that may require surgical repair.
Causes
As ?overuse? disorders, Achilles tendonitis and tendonosis are usually caused by a sudden increase of a repetitive activity involving the Achilles tendon. Such activity puts too much stress on the tendon too quickly, leading to micro-injury of the tendon fibers. Due to this ongoing stress on the tendon, the body is unable to repair the injured tissue. The structure of the tendon is then altered, resulting in continued pain. Achilles4Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis and tendonosis are also common in individuals whose work puts stress on their ankles and feet, such as laborers, as well as in ?weekend warriors?-those who are less conditioned and participate in athletics only on weekends or infrequently. In addition, people with excessive pronation (flattening of the arch) have a tendency to develop Achilles tendonitis and tendonosis due to the greater demands placed on the tendon when walking. If these individuals wear shoes without adequate stability, their over-pronation could further aggravate the Achilles tendon.
Symptoms
Pain in the back of the heel that can be a shooting pain, burning pain or even an intense piercing pain. Swelling, tenderness and warmth over the Achilles tendon especially at the insertion of the tendon to the calcaneous, which may even extend into the muscle of the calf. Difficulty walking, sometimes the pain makes walking impossible. Pain that is aggravated by activities that repeatedly stress the tendon, causing inflammation or pain that occurs in the first few steps of the morning or after sitting down for extended periods of time which gets better with mild activity. It is important to note though that achilles tendinosis can develop gradually without a history of trauma.
Diagnosis
Physicians usually pinch your Achilles tendon with their fingers to test for swelling and pain. If the tendon itself is inflamed, your physician may be able to feel warmth and swelling around the tissue, or, in chronic cases, lumps of scar tissue. You will probably be asked to walk around the exam room so your physician can examine your stride. To check for complete rupture of the tendon, your physician may perform the Thompson test. Your physician squeezes your calf; if your Achilles is not torn, the foot will point downward. If your Achilles is torn, the foot will remain in the same position. Should your physician require a closer look, these imaging tests may be performed. X-rays taken from different angles may be used to rule out other problems, such as ankle fractures. MRI (magnetic resonance imaging) uses magnetic waves to create pictures of your ankle that let physicians more clearly look at the tendons surrounding your ankle joint.
Nonsurgical Treatment
Many physical therapies exist to help with the pain. We have found the combination of modalities, stretching, acupuncture, footwear modification and myofascial release to be very effective. In resilient cases, a promising new treatment called Radial Shockwave may be indicated. The key to the treatment of this, and other foot problems, is an accurate diagnosis. With this, a treatment regimen tailored to you and your specific situation can be devised. We treat many acute and chronic achilles tendinitis in Edmonton and St. Albert, so remember ?it shouldn?t hurt.?

Surgical Treatment
If non-surgical approaches fail to restore the tendon to its normal condition, surgery may be necessary. The foot and ankle surgeon will select the best procedure to repair the tendon, based upon the extent of the injury, the patient?s age and activity level, and other factors.
Prevention
Wear shoes that fit correctly and support your feet: Replace your running or exercise shoes before the padding or shock absorption wears out. Shock absorption greatly decreases as the treads on the bottoms or sides of your shoes begin to wear down. You may need running shoes that give your foot more heel or arch support. You may need shoe inserts to keep your foot from rolling inward. Stretch before you exercise: Always warm up your muscles and stretch gently before you exercise. Do cool down exercises when you are finished. This will loosen your muscles and decrease stress on your Achilles tendon. Exercise the right way: If your tendinitis is caused by the way that you exercise, ask a trainer, coach, or your caregiver for help. They can teach you ways to train or exercise to help prevent Achilles tendinitis. Do not run or exercise on uneven or hard surfaces. Instead, run on softer surfaces such as treadmills, rubber tracks, grass, or evenly packed dirt tracks.
 Achilles Tendinitis is a common overuse injury which results in inflammation of the achilles tendon, most frequently causing mild to severe heel pain. The achilles tendon is the largest tendon in the body, connecting your calf muscle to your heel bone. It?s used with every step - when you walk, run, and jump. Although the Achilles tendon can withstand great stresses, it?s also prone to tendinitis. The condition is very common in athletes, especially runners who?ve suddenly increased the intensity or duration of their workouts. It?s also common in middle-aged, ?weekend athletes? who play sports like tennis or basketball only occasionally. The pain from achilles tendinitis may be felt anywhere from the back of the leg to the top of the heel. Most cases are mild and can be treated at home under a podiatrist?s supervision. Severe cases of Achilles tendinitis can lead to tendon tears (ruptures) that may require surgical repair.
Achilles Tendinitis is a common overuse injury which results in inflammation of the achilles tendon, most frequently causing mild to severe heel pain. The achilles tendon is the largest tendon in the body, connecting your calf muscle to your heel bone. It?s used with every step - when you walk, run, and jump. Although the Achilles tendon can withstand great stresses, it?s also prone to tendinitis. The condition is very common in athletes, especially runners who?ve suddenly increased the intensity or duration of their workouts. It?s also common in middle-aged, ?weekend athletes? who play sports like tennis or basketball only occasionally. The pain from achilles tendinitis may be felt anywhere from the back of the leg to the top of the heel. Most cases are mild and can be treated at home under a podiatrist?s supervision. Severe cases of Achilles tendinitis can lead to tendon tears (ruptures) that may require surgical repair.
Causes
As ?overuse? disorders, Achilles tendonitis and tendonosis are usually caused by a sudden increase of a repetitive activity involving the Achilles tendon. Such activity puts too much stress on the tendon too quickly, leading to micro-injury of the tendon fibers. Due to this ongoing stress on the tendon, the body is unable to repair the injured tissue. The structure of the tendon is then altered, resulting in continued pain. Achilles4Athletes are at high risk for developing disorders of the Achilles tendon. Achilles tendonitis and tendonosis are also common in individuals whose work puts stress on their ankles and feet, such as laborers, as well as in ?weekend warriors?-those who are less conditioned and participate in athletics only on weekends or infrequently. In addition, people with excessive pronation (flattening of the arch) have a tendency to develop Achilles tendonitis and tendonosis due to the greater demands placed on the tendon when walking. If these individuals wear shoes without adequate stability, their over-pronation could further aggravate the Achilles tendon.
Symptoms
Pain in the back of the heel that can be a shooting pain, burning pain or even an intense piercing pain. Swelling, tenderness and warmth over the Achilles tendon especially at the insertion of the tendon to the calcaneous, which may even extend into the muscle of the calf. Difficulty walking, sometimes the pain makes walking impossible. Pain that is aggravated by activities that repeatedly stress the tendon, causing inflammation or pain that occurs in the first few steps of the morning or after sitting down for extended periods of time which gets better with mild activity. It is important to note though that achilles tendinosis can develop gradually without a history of trauma.
Diagnosis
Physicians usually pinch your Achilles tendon with their fingers to test for swelling and pain. If the tendon itself is inflamed, your physician may be able to feel warmth and swelling around the tissue, or, in chronic cases, lumps of scar tissue. You will probably be asked to walk around the exam room so your physician can examine your stride. To check for complete rupture of the tendon, your physician may perform the Thompson test. Your physician squeezes your calf; if your Achilles is not torn, the foot will point downward. If your Achilles is torn, the foot will remain in the same position. Should your physician require a closer look, these imaging tests may be performed. X-rays taken from different angles may be used to rule out other problems, such as ankle fractures. MRI (magnetic resonance imaging) uses magnetic waves to create pictures of your ankle that let physicians more clearly look at the tendons surrounding your ankle joint.
Nonsurgical Treatment
Many physical therapies exist to help with the pain. We have found the combination of modalities, stretching, acupuncture, footwear modification and myofascial release to be very effective. In resilient cases, a promising new treatment called Radial Shockwave may be indicated. The key to the treatment of this, and other foot problems, is an accurate diagnosis. With this, a treatment regimen tailored to you and your specific situation can be devised. We treat many acute and chronic achilles tendinitis in Edmonton and St. Albert, so remember ?it shouldn?t hurt.?

Surgical Treatment
If non-surgical approaches fail to restore the tendon to its normal condition, surgery may be necessary. The foot and ankle surgeon will select the best procedure to repair the tendon, based upon the extent of the injury, the patient?s age and activity level, and other factors.
Prevention
Wear shoes that fit correctly and support your feet: Replace your running or exercise shoes before the padding or shock absorption wears out. Shock absorption greatly decreases as the treads on the bottoms or sides of your shoes begin to wear down. You may need running shoes that give your foot more heel or arch support. You may need shoe inserts to keep your foot from rolling inward. Stretch before you exercise: Always warm up your muscles and stretch gently before you exercise. Do cool down exercises when you are finished. This will loosen your muscles and decrease stress on your Achilles tendon. Exercise the right way: If your tendinitis is caused by the way that you exercise, ask a trainer, coach, or your caregiver for help. They can teach you ways to train or exercise to help prevent Achilles tendinitis. Do not run or exercise on uneven or hard surfaces. Instead, run on softer surfaces such as treadmills, rubber tracks, grass, or evenly packed dirt tracks.
Torn Achilles Tendon Brace
Overview
 Achilles tendonitis is an inflammation of the Achilles tendon, which attaches the calf muscles (gastrocnemius and soleus) to the heel bone (calcaneus). Pain can be felt on the back of the heel at the attachment of the tendon, along the length of the tendon, or at the base of the calf where the tendon attaches to the muscle. Swelling is not always present with this injury, but it may occur in severe cases.
Achilles tendonitis is an inflammation of the Achilles tendon, which attaches the calf muscles (gastrocnemius and soleus) to the heel bone (calcaneus). Pain can be felt on the back of the heel at the attachment of the tendon, along the length of the tendon, or at the base of the calf where the tendon attaches to the muscle. Swelling is not always present with this injury, but it may occur in severe cases.
Causes
A lot of stress on the feet is the cause of Achilles tendinitis. It is a common athletic injury. Things that can cause tendinitis include, pushing your body too fast and too soon, sudden increase in activity, sports that cause you to quickly start and stop, poor fitting shoes, bad footwear, severe injury to the Achilles tendon, running or exercising on uneven ground, running uphill, tight calf muscles, bone spur (extra bone growth in heel that rubs the tendon and causes pain), flat arches, feet that roll in (overpronation), and weak calf muscles, not warming up before exercising.
Symptoms
The most common site of Achilles Tendonitis is at the heel to 4 inches above the heel. The diagnosis of this problem is made when the following signs are present. Pain in the Achilles tendon with up and down movement of the foot at the ankle. Pain in the Achilles tendon when you squeeze the tendon from side to side. If you are unable to move the foot either up or down, or you have intense pain when trying to walk, you may have a tear of the Achilles tendon, and you should see a doctor immediately. Also if you have severe pain in the calf, with or without discolorations of the skin, you may have a blood clot, and this is a medical emergency; see a doctor immediately. If you do not fall into either of these categories then try the following suggestions.
Diagnosis
If you think you have Achilles tendinitis, make an appointment to see your doctor. The doctor will ask you questions about your recent activity and look for signs. The foot not flexing when the calf muscle is pressed ( if Achilles ruptures or tears in half). Swelling on the back of the foot. Pain in the back of the foot. Limited range of motion in ankle. An X-ray or MRI scan can check for tendinitis.
Nonsurgical Treatment
Massage therapy improves blood flow to the muscles and tissues of the affected area while increasing range of motion and can prevent recurring injury. The healing process can be quickened using ultrasound heat therapy to improve blood flow to the affected area. Wearing a night brace keeps the leg flexed, preventing stiffening of the tendon, which would impair healing. Stretching exercises increase flexibility and allow the tendon to heal without shortening, a deformity resulting in chronic pain. Persistent Achilles pain may warrant the use of a cast or walking boot to be worn for 4-6 weeks stabilizing the tendon so it can heal. After removal of the cast or boot, physical therapy will be ordered to increase functionality of the affected limb. To reduce chronic inflammation of the tendon, corticosteroid injections may be prescribed. It?s important to note that this corticosteroid treatment increases the risk of tendon rupture. Ultrasound imaging may be used by the physician administering the steroid injection, in order to help visualize the affected area. When all other therapies have failed to or tendon rupture occurs, surgical intervention and repair of the muscles and tendons is the last treatment option.

Surgical Treatment
If several months of more-conservative treatments don't work or if the tendon has torn, your doctor may suggest surgery to repair your Achilles tendon.
Prevention
Do strengthening and stretching exercises to keep calf muscles strong and flexible. Keep your hamstring muscles flexible by stretching. Warm up and stretch adequately before participating in any sports. Always increase the intensity and duration of training gradually. Do not continue an exercise if you experience pain over the tendon. Wear properly fitted running and other sports shoes, including properly fitted arch supports if your feet roll inwards excessively (over-pronate).
 Achilles tendonitis is an inflammation of the Achilles tendon, which attaches the calf muscles (gastrocnemius and soleus) to the heel bone (calcaneus). Pain can be felt on the back of the heel at the attachment of the tendon, along the length of the tendon, or at the base of the calf where the tendon attaches to the muscle. Swelling is not always present with this injury, but it may occur in severe cases.
Achilles tendonitis is an inflammation of the Achilles tendon, which attaches the calf muscles (gastrocnemius and soleus) to the heel bone (calcaneus). Pain can be felt on the back of the heel at the attachment of the tendon, along the length of the tendon, or at the base of the calf where the tendon attaches to the muscle. Swelling is not always present with this injury, but it may occur in severe cases.
Causes
A lot of stress on the feet is the cause of Achilles tendinitis. It is a common athletic injury. Things that can cause tendinitis include, pushing your body too fast and too soon, sudden increase in activity, sports that cause you to quickly start and stop, poor fitting shoes, bad footwear, severe injury to the Achilles tendon, running or exercising on uneven ground, running uphill, tight calf muscles, bone spur (extra bone growth in heel that rubs the tendon and causes pain), flat arches, feet that roll in (overpronation), and weak calf muscles, not warming up before exercising.
Symptoms
The most common site of Achilles Tendonitis is at the heel to 4 inches above the heel. The diagnosis of this problem is made when the following signs are present. Pain in the Achilles tendon with up and down movement of the foot at the ankle. Pain in the Achilles tendon when you squeeze the tendon from side to side. If you are unable to move the foot either up or down, or you have intense pain when trying to walk, you may have a tear of the Achilles tendon, and you should see a doctor immediately. Also if you have severe pain in the calf, with or without discolorations of the skin, you may have a blood clot, and this is a medical emergency; see a doctor immediately. If you do not fall into either of these categories then try the following suggestions.
Diagnosis
If you think you have Achilles tendinitis, make an appointment to see your doctor. The doctor will ask you questions about your recent activity and look for signs. The foot not flexing when the calf muscle is pressed ( if Achilles ruptures or tears in half). Swelling on the back of the foot. Pain in the back of the foot. Limited range of motion in ankle. An X-ray or MRI scan can check for tendinitis.
Nonsurgical Treatment
Massage therapy improves blood flow to the muscles and tissues of the affected area while increasing range of motion and can prevent recurring injury. The healing process can be quickened using ultrasound heat therapy to improve blood flow to the affected area. Wearing a night brace keeps the leg flexed, preventing stiffening of the tendon, which would impair healing. Stretching exercises increase flexibility and allow the tendon to heal without shortening, a deformity resulting in chronic pain. Persistent Achilles pain may warrant the use of a cast or walking boot to be worn for 4-6 weeks stabilizing the tendon so it can heal. After removal of the cast or boot, physical therapy will be ordered to increase functionality of the affected limb. To reduce chronic inflammation of the tendon, corticosteroid injections may be prescribed. It?s important to note that this corticosteroid treatment increases the risk of tendon rupture. Ultrasound imaging may be used by the physician administering the steroid injection, in order to help visualize the affected area. When all other therapies have failed to or tendon rupture occurs, surgical intervention and repair of the muscles and tendons is the last treatment option.

Surgical Treatment
If several months of more-conservative treatments don't work or if the tendon has torn, your doctor may suggest surgery to repair your Achilles tendon.
Prevention
Do strengthening and stretching exercises to keep calf muscles strong and flexible. Keep your hamstring muscles flexible by stretching. Warm up and stretch adequately before participating in any sports. Always increase the intensity and duration of training gradually. Do not continue an exercise if you experience pain over the tendon. Wear properly fitted running and other sports shoes, including properly fitted arch supports if your feet roll inwards excessively (over-pronate).
What Can You Do About Fallen Arches?
Overview
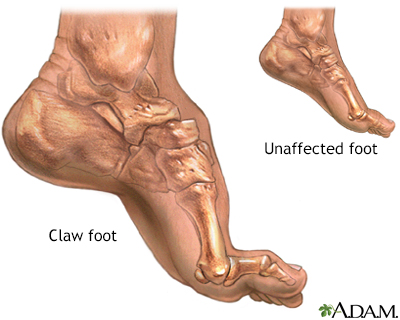
Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
There are several factors that can contribute to the development of fallen arches. These factors include the following. Genetic abnormality, torn or stretched tendons, amage to the posterior tibial tendon, bone fractures, dislocation of bones, nerve damage, rheumatoid arthritis and other medical conditions. In addition, there are other factors that can increase your risk of developing fallen arches. These risk factors include diabetes, pregnancy, Obesity and Aging.
Symptoms
Flat feet may not cause any symptoms at all. Rigid flat feet may cause pain, calluses, blisters, or skin redness on the inner side of the foot. A stiff foot, weakness or numbness of the foot, Rapid wearing out of shoes-worn shoes lean in toward each other. Difficulty or pain with activities like running-in the foot, knee or hip.
Diagnosis
Many medical professionals can diagnose a flat foot by examining the patient standing or just looking at them. On going up onto tip toe the deformity will correct when this is a flexible flat foot in a child with lax joints. Such correction is not seen in the adult with a rigid flat foot. An easy and traditional home diagnosis is the "wet footprint" test, performed by wetting the feet in water and then standing on a smooth, level surface such as smooth concrete or thin cardboard or heavy paper. Usually, the more the sole of the foot that makes contact (leaves a footprint), the flatter the foot. In more extreme cases, known as a kinked flatfoot, the entire inner edge of the footprint may actually bulge outward, where in a normal to high arch this part of the sole of the foot does not make contact with the ground at all.
Non Surgical Treatment
Treatment of flat feet may be appropriate if there is associated foot or lower leg pain, or if the condition affects the knees or the lower back. Treatment may include using Orthoses such as an arch support, foot gymnastics or other exercises as recommended by a podiatrist/orthotist or physical therapist. In cases of severe flat feet, orthoses should be used through a gradual process to lessen discomfort. Over several weeks, slightly more material is added to the orthosis to raise the arch. These small changes allow the foot structure to adjust gradually, as well as giving the patient time to acclimatise to the sensation of wearing orthoses. Once prescribed, orthoses are generally worn for the rest of the patient's life. In some cases, surgery can provide lasting relief, and even create an arch where none existed before; it should be considered a last resort, as it is usually very time consuming and costly.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.

Fallen arches or flat feet is a condition in which the arch or instep of the foot collapses and comes in contact with the ground. In some individuals, this arch never develops while they are growing. Flat feet (also called pes planus or fallen arches) is a formal reference to a medical condition in which the arch of the foot collapses, with the entire sole of the foot coming into complete or near-complete contact with the ground. In some individuals (an estimated 20-30% of the general population) the arch simply never develops in one foot (unilaterally) or both feet (bilaterally).
Causes
There are several factors that can contribute to the development of fallen arches. These factors include the following. Genetic abnormality, torn or stretched tendons, amage to the posterior tibial tendon, bone fractures, dislocation of bones, nerve damage, rheumatoid arthritis and other medical conditions. In addition, there are other factors that can increase your risk of developing fallen arches. These risk factors include diabetes, pregnancy, Obesity and Aging.
Symptoms
Flat feet may not cause any symptoms at all. Rigid flat feet may cause pain, calluses, blisters, or skin redness on the inner side of the foot. A stiff foot, weakness or numbness of the foot, Rapid wearing out of shoes-worn shoes lean in toward each other. Difficulty or pain with activities like running-in the foot, knee or hip.
Diagnosis
Many medical professionals can diagnose a flat foot by examining the patient standing or just looking at them. On going up onto tip toe the deformity will correct when this is a flexible flat foot in a child with lax joints. Such correction is not seen in the adult with a rigid flat foot. An easy and traditional home diagnosis is the "wet footprint" test, performed by wetting the feet in water and then standing on a smooth, level surface such as smooth concrete or thin cardboard or heavy paper. Usually, the more the sole of the foot that makes contact (leaves a footprint), the flatter the foot. In more extreme cases, known as a kinked flatfoot, the entire inner edge of the footprint may actually bulge outward, where in a normal to high arch this part of the sole of the foot does not make contact with the ground at all.
Non Surgical Treatment
Treatment of flat feet may be appropriate if there is associated foot or lower leg pain, or if the condition affects the knees or the lower back. Treatment may include using Orthoses such as an arch support, foot gymnastics or other exercises as recommended by a podiatrist/orthotist or physical therapist. In cases of severe flat feet, orthoses should be used through a gradual process to lessen discomfort. Over several weeks, slightly more material is added to the orthosis to raise the arch. These small changes allow the foot structure to adjust gradually, as well as giving the patient time to acclimatise to the sensation of wearing orthoses. Once prescribed, orthoses are generally worn for the rest of the patient's life. In some cases, surgery can provide lasting relief, and even create an arch where none existed before; it should be considered a last resort, as it is usually very time consuming and costly.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.
Ways To Diagnose Fallen Arches
Overview

A person with flat feet (fallen arches) has low arches or no arches at all. Most cases don't cause problems and treatment isn't usually needed. The arch, or instep, is the inside part of the foot that's usually raised off the ground when you stand, while the rest of the foot remains flat on the ground. Most people have a noticeable space on the inner part of their foot (the arch). The height of the arch varies from person to person.
Causes
Generally fallen arches are a condition inherited from one or both parents. In addition, age, obesity, and pregnancy cause our arches to collapse. Being in a job that requires long hours of standing and/or walking (e.g. teaching, retail, hospitality, building etc) contributes to this condition, especially when standing on hard surfaces like concrete floors. Last, but not least unsupportive footwear makes our feet roll in more than they should.
Symptoms
Depending on the cause of the flatfoot, a patient may experience one or more of the different symptoms below. Pain along the course of the posterior tibial tendon which lies on the inside of the foot and ankle. This can be associated with swelling on the inside of the ankle. Pain that is worse with activity. High intensity or impact activities, such as running, can be very difficult. Some patients can have difficulty walking or even standing for long periods of time. When the foot collapses, the heel bone may shift position and put pressure on the outside ankle bone (fibula). This can cause pain on the outside of the ankle. Arthritis in the heel also causes this same type of pain. Patients with an old injury or arthritis in the middle of the foot can have painful, bony bumps on the top and inside of the foot. These make shoewear very difficult. Occasionally, the bony spurs are so large that they pinch the nerves which can result in numbness and tingling on the top of the foot and into the toes. Diabetics may only notice swelling or a large bump on the bottom of the foot. Because their sensation is affected, people with diabetes may not have any pain. The large bump can cause skin problems and an ulcer (a sore that does not heal) may develop if proper diabetic shoewear is not used.
Diagnosis
Your doctor will ask about your symptoms and medical history. A physical and foot exam will be done. Flat feet can be diagnosed by appearance. To determine if the foot is rigid, you may be asked to do some simple tasks.
Non Surgical Treatment
Some patients with flat feet may automatically align their limbs in such a way that unpleasant symptoms never develop. In such cases treatment is not usually required. Pain in the foot that is caused by flat feet may be alleviated if the patient wears supportive well-fitted shoes. Some patients say that symptoms improve with extra-wide fitting shoes. Fitted insoles or orthotics (custom-designed arch supports) may relieve pressure from the arch and reduce pain if the patient's feet roll or over-pronate. The benefits of an orthotic only exist while it is being worn. Patients with tendonitis of the posterior tibial tendon may benefit if a wedge is inserted along the inside edge of the orthotic - this takes some of the load off the tendon tissue. Wearing an ankle brace may help patients with posterior tibial tendinitis, until the inflammation comes down. Rest, doctors may advise some patients to rest and avoid activities which may make the foot (feet) feel worse, until the foot (feet) feels better. A combination of an insole and some kind of painkiller may help patients with a ruptured tendon, as well as those with arthritis. Patients with a ruptured tendon or arthritis who find insoles with painkillers ineffective may require surgical intervention. Patients, usually children, whose bones did not or are not developing properly, resulting in flat feet from birth, may require surgical intervention to separate fused bones (rare). Bodyweight management, if the patient is obese the doctor may advise him/her to lose weight. A significant number of obese patients with flat feet who successfully lose weight experience considerable improvement of symptoms.
Surgical Treatment

Procedures may include the following. Fusing foot or ankle bones together (arthrodesis). Removing bones or bony growths, also called spurs (excision). Cutting or changing the shape of the bone (osteotomy). Cleaning the tendons' protective coverings (synovectomy). Adding tendon from other parts of your body to tendons in your foot to help balance the "pull" of the tendons and form an arch (tendon transfer). Grafting bone to your foot to make the arch rise more naturally (lateral column lengthening).
Prevention
Donning a first-rate pair of arch supports, therapeutic socks and proper footwear before heading out to enjoy hours of holiday fun is one option to consider. Your podiatrist can help you find just the right ones. Once you have them on, they?ll help ease the amount of pressure being put on your body and keep the blood flowing in the right direction. While you?re standing in line, consider doing a bit of exercise as well. We?re not talking about channeling your inner Jack LaLanne here. Otherwise, you might attract the attention of the mall security guards. Simple ankle rotations and walking in place may help to reduce edema and give your flat feet a bit of a break. If you happen to be in a shopping mall or center where foot massages are available, take advantage of them periodically. They are likely to make you feel better and it?s a great excuse to carve out a few quiet moments for yourself. If you can?t visit a professional, tuck a personal foot massager into your purse. That way, you can lightly massage your own feet during the car ride home. Lastly, there are certain foods and nutritional supplements available that may reduce edema caused by standing on flat feet for hours at a time. The list includes potassium rich foods like raisins, bananas, baby carrots, nuts and yogurt. So, you may want to pack a snack for those trips to the mall or hit the food court before you hit the stores.

A person with flat feet (fallen arches) has low arches or no arches at all. Most cases don't cause problems and treatment isn't usually needed. The arch, or instep, is the inside part of the foot that's usually raised off the ground when you stand, while the rest of the foot remains flat on the ground. Most people have a noticeable space on the inner part of their foot (the arch). The height of the arch varies from person to person.
Causes
Generally fallen arches are a condition inherited from one or both parents. In addition, age, obesity, and pregnancy cause our arches to collapse. Being in a job that requires long hours of standing and/or walking (e.g. teaching, retail, hospitality, building etc) contributes to this condition, especially when standing on hard surfaces like concrete floors. Last, but not least unsupportive footwear makes our feet roll in more than they should.
Symptoms
Depending on the cause of the flatfoot, a patient may experience one or more of the different symptoms below. Pain along the course of the posterior tibial tendon which lies on the inside of the foot and ankle. This can be associated with swelling on the inside of the ankle. Pain that is worse with activity. High intensity or impact activities, such as running, can be very difficult. Some patients can have difficulty walking or even standing for long periods of time. When the foot collapses, the heel bone may shift position and put pressure on the outside ankle bone (fibula). This can cause pain on the outside of the ankle. Arthritis in the heel also causes this same type of pain. Patients with an old injury or arthritis in the middle of the foot can have painful, bony bumps on the top and inside of the foot. These make shoewear very difficult. Occasionally, the bony spurs are so large that they pinch the nerves which can result in numbness and tingling on the top of the foot and into the toes. Diabetics may only notice swelling or a large bump on the bottom of the foot. Because their sensation is affected, people with diabetes may not have any pain. The large bump can cause skin problems and an ulcer (a sore that does not heal) may develop if proper diabetic shoewear is not used.
Diagnosis
Your doctor will ask about your symptoms and medical history. A physical and foot exam will be done. Flat feet can be diagnosed by appearance. To determine if the foot is rigid, you may be asked to do some simple tasks.
Non Surgical Treatment
Some patients with flat feet may automatically align their limbs in such a way that unpleasant symptoms never develop. In such cases treatment is not usually required. Pain in the foot that is caused by flat feet may be alleviated if the patient wears supportive well-fitted shoes. Some patients say that symptoms improve with extra-wide fitting shoes. Fitted insoles or orthotics (custom-designed arch supports) may relieve pressure from the arch and reduce pain if the patient's feet roll or over-pronate. The benefits of an orthotic only exist while it is being worn. Patients with tendonitis of the posterior tibial tendon may benefit if a wedge is inserted along the inside edge of the orthotic - this takes some of the load off the tendon tissue. Wearing an ankle brace may help patients with posterior tibial tendinitis, until the inflammation comes down. Rest, doctors may advise some patients to rest and avoid activities which may make the foot (feet) feel worse, until the foot (feet) feels better. A combination of an insole and some kind of painkiller may help patients with a ruptured tendon, as well as those with arthritis. Patients with a ruptured tendon or arthritis who find insoles with painkillers ineffective may require surgical intervention. Patients, usually children, whose bones did not or are not developing properly, resulting in flat feet from birth, may require surgical intervention to separate fused bones (rare). Bodyweight management, if the patient is obese the doctor may advise him/her to lose weight. A significant number of obese patients with flat feet who successfully lose weight experience considerable improvement of symptoms.
Surgical Treatment
Procedures may include the following. Fusing foot or ankle bones together (arthrodesis). Removing bones or bony growths, also called spurs (excision). Cutting or changing the shape of the bone (osteotomy). Cleaning the tendons' protective coverings (synovectomy). Adding tendon from other parts of your body to tendons in your foot to help balance the "pull" of the tendons and form an arch (tendon transfer). Grafting bone to your foot to make the arch rise more naturally (lateral column lengthening).
Prevention
Donning a first-rate pair of arch supports, therapeutic socks and proper footwear before heading out to enjoy hours of holiday fun is one option to consider. Your podiatrist can help you find just the right ones. Once you have them on, they?ll help ease the amount of pressure being put on your body and keep the blood flowing in the right direction. While you?re standing in line, consider doing a bit of exercise as well. We?re not talking about channeling your inner Jack LaLanne here. Otherwise, you might attract the attention of the mall security guards. Simple ankle rotations and walking in place may help to reduce edema and give your flat feet a bit of a break. If you happen to be in a shopping mall or center where foot massages are available, take advantage of them periodically. They are likely to make you feel better and it?s a great excuse to carve out a few quiet moments for yourself. If you can?t visit a professional, tuck a personal foot massager into your purse. That way, you can lightly massage your own feet during the car ride home. Lastly, there are certain foods and nutritional supplements available that may reduce edema caused by standing on flat feet for hours at a time. The list includes potassium rich foods like raisins, bananas, baby carrots, nuts and yogurt. So, you may want to pack a snack for those trips to the mall or hit the food court before you hit the stores.
Pain In The Foot's Arch Everything You Need To Learn
Overview
A person with flat feet (fallen arches) has low arches or no arches at all. Most cases don't cause problems and treatment isn't usually needed. The arch, or instep, is the inside part of the foot that's usually raised off the ground when you stand, while the rest of the foot remains flat on the ground. Most people have a noticeable space on the inner part of their foot (the arch). The height of the arch varies from person to person.

Causes
Over-stretching or tearing the arch pad causes the dull ache that is associated with arch pain. Pain is most keenly felt when weight is put onto the foot, or when pushing off the foot into the next stride. The pain of foot arch strain can be particularly acute after sitting for a long time, or when getting up in the morning. Those most susceptible to the condition are people with very high, rigid arches. The injury is also common in middle-aged people who have been inactive for a long period of time before suddenly increasing their physical activity. The injury is particularly common in runners and joggers.
Symptoms
Symptoms of arch pain and arch strain are found in the underside of the foot, where the foot arch is. Arch pain and arch strain is actually inflammation of the tissue in the midfoot, formed by a band that stretches from the toes to the heel. The arch of the foot is needed for the proper transfer of weight from the heel to toe. When the band forming the arch of the foot or plantar fascia becomes inflamed, it becomes painful to perform simple tasks.
Diagnosis
Flat feet are easy to identify while standing or walking. When someone with flat feet stands, their inner foot or arch flattens and their foot may roll over to the inner side. This is known as overpronation. To see whether your foot overpronates, stand on tiptoes or push your big toe back as far as possible. If the arch of your foot doesn't appear, your foot is likely to overpronate when you walk or run. It can be difficult to tell whether a child has flat feet because their arches may not fully develop until they're 10 years of age.
Non Surgical Treatment
High arches that are flexible do not require any treatment. In cases where there is pain, shoe modifications such as an arch insert or support insole can help to relieve pain during walking. Custom orthotic devices can be given that fit into the shoe and provide stability and cushioning effect. Your doctor may recommend a brace to help keep the foot and ankle stable. In severe cases, surgery is performed to flatten the foot. Any coexisting nerve disorders are also treated.

Surgical Treatment
In rare cases, surgery may be needed if a child has flat feet caused by a problem they're born with (a congenital abnormality). The foot may need to be straightened or the bones may need to be separated if they're fused together. Painkillers and insoles are the first treatment options for flat feet that are caused by a joint problem, such as arthritis or a torn tendon. However, surgery may be recommended if the injury or condition is severely affecting your feet. Where flat feet are caused by a condition that affects the nervous system, special shoes, insoles, or supportive foot or leg braces may be needed. Again, in severe cases, an operation may be needed to straighten the feet.
Stretching Exercises
Below are two simple plantar fasciitis stretching exercises to help improve the flexibility of the muscles and tendons around the foot and ankle. Plantar fasciitis stretch taken from The Stretching Handbook. Kneel on one foot and place your body weight over your knee. Keep your heel on the ground and lean forward. In the photo to the left, the athlete is stretching the arch of her left foot. Kneel on one foot with your hands on the ground. Place your body weight over your knee and slowly move your knee forward. Keep your toes on the ground and arch your foot. In the photo to the right, the athlete is stretching the arch of his right foot.
A person with flat feet (fallen arches) has low arches or no arches at all. Most cases don't cause problems and treatment isn't usually needed. The arch, or instep, is the inside part of the foot that's usually raised off the ground when you stand, while the rest of the foot remains flat on the ground. Most people have a noticeable space on the inner part of their foot (the arch). The height of the arch varies from person to person.

Causes
Over-stretching or tearing the arch pad causes the dull ache that is associated with arch pain. Pain is most keenly felt when weight is put onto the foot, or when pushing off the foot into the next stride. The pain of foot arch strain can be particularly acute after sitting for a long time, or when getting up in the morning. Those most susceptible to the condition are people with very high, rigid arches. The injury is also common in middle-aged people who have been inactive for a long period of time before suddenly increasing their physical activity. The injury is particularly common in runners and joggers.
Symptoms
Symptoms of arch pain and arch strain are found in the underside of the foot, where the foot arch is. Arch pain and arch strain is actually inflammation of the tissue in the midfoot, formed by a band that stretches from the toes to the heel. The arch of the foot is needed for the proper transfer of weight from the heel to toe. When the band forming the arch of the foot or plantar fascia becomes inflamed, it becomes painful to perform simple tasks.
Diagnosis
Flat feet are easy to identify while standing or walking. When someone with flat feet stands, their inner foot or arch flattens and their foot may roll over to the inner side. This is known as overpronation. To see whether your foot overpronates, stand on tiptoes or push your big toe back as far as possible. If the arch of your foot doesn't appear, your foot is likely to overpronate when you walk or run. It can be difficult to tell whether a child has flat feet because their arches may not fully develop until they're 10 years of age.
Non Surgical Treatment
High arches that are flexible do not require any treatment. In cases where there is pain, shoe modifications such as an arch insert or support insole can help to relieve pain during walking. Custom orthotic devices can be given that fit into the shoe and provide stability and cushioning effect. Your doctor may recommend a brace to help keep the foot and ankle stable. In severe cases, surgery is performed to flatten the foot. Any coexisting nerve disorders are also treated.

Surgical Treatment
In rare cases, surgery may be needed if a child has flat feet caused by a problem they're born with (a congenital abnormality). The foot may need to be straightened or the bones may need to be separated if they're fused together. Painkillers and insoles are the first treatment options for flat feet that are caused by a joint problem, such as arthritis or a torn tendon. However, surgery may be recommended if the injury or condition is severely affecting your feet. Where flat feet are caused by a condition that affects the nervous system, special shoes, insoles, or supportive foot or leg braces may be needed. Again, in severe cases, an operation may be needed to straighten the feet.
Stretching Exercises
Below are two simple plantar fasciitis stretching exercises to help improve the flexibility of the muscles and tendons around the foot and ankle. Plantar fasciitis stretch taken from The Stretching Handbook. Kneel on one foot and place your body weight over your knee. Keep your heel on the ground and lean forward. In the photo to the left, the athlete is stretching the arch of her left foot. Kneel on one foot with your hands on the ground. Place your body weight over your knee and slowly move your knee forward. Keep your toes on the ground and arch your foot. In the photo to the right, the athlete is stretching the arch of his right foot.
Pain In The Arch Causes Symptoms And Treatments
Overview
Plantar fasciitis is a common and often persistent kind of repetitive strain injury afflicting runners, walkers and hikers, and nearly anyone who stands for a living, cashiers, for instance. It causes mainly foot arch pain and/or heel pain. Morning foot pain is a signature symptom. Plantar fasciitis is not the same thing as heel spurs and flat feet, but they are related and often confused. Most people recover from plantar fasciitis with a little rest, arch support (regular shoe inserts or just comfy shoes), and stretching, but not everyone. Severe cases can stop you in your tracks, undermine your fitness and general health, and drag on for years.

Causes
In most cases, plantar fasciitis develops without a specific, identifiable reason. There are, however, many factors that can make you more prone to the condition. Tighter calf muscles that make it difficult to flex your foot and bring your toes up toward your shin. Obesity. Very high arch. Repetitive impact activity (running/sports). New or increased activity.Although many people with plantar fasciitis have heel spurs, spurs are not the cause of plantar fasciitis pain. One out of 10 people has heel spurs, but only 1 out of 20 people (5%) with heel spurs has foot pain. Because the spur is not the cause of plantar fasciitis, the pain can be treated without removing the spur.
Symptoms
The primary symptom is pain or aching in the arch area. This can be accompanied by inflammation and tenderness. If the pain is caused by the plantar fascia, it is likely to be considerably more severe in the mornings due to the muscles being unused. If you notice that the twinges of pain you have are most commonly associated with or immediately after exercise, you might want to visit a good athletic shoe store to make sure you are wearing the right kind of shoe. Another cause of arch pain is plantar fasciitis. The plantar fascia is a tough tissue structure that holds the bottom part of the arch in place. The fascia often becomes inflamed and sore, usually as a result of repetitive motion (for example, very common in those who stand on their feet for work). The pain is often noticeable first thing in the morning and worse with activity.
Diagnosis
To come to a correct diagnosis, your podiatrist will examine your foot by using his or her fingers to look for a lump or stone bruise in the ball of your foot. He or she will examine your foot to look for deformities such as high or low arches, or to see if you have hammertoes. He or she may use x-rays, MRIs (magnetic resource imaging), and CT scans to rule out fractures and damage to ligaments, tendons, and other surrounding tissues. Your doctor will also inquire about your daily activities, symptoms, medical history, and family history. If you spend a lot of time running or jumping, you may be at a higher risk for pain in the bottom of your foot. These diagnostic tests will help your doctor come to a proper diagnosis and create an appropriate treatment plan.
Non Surgical Treatment
There are many different causes of and treatments for flat foot. The most important part of treatment is determining the exact flat foot type on an individual basis, and doing so early on. The main objective is to become educated on the potential problems, so that you can stop them before they start. Conservative treatment is often successful if initiated early. The old adage "a stitch in time saves nine" definitely applies to the human body, hopefully more figuratively than literally. Do not ignore what your common sense and your body are telling you. Yes, you can live without an arch, but never neglect a symptomatic foot. If you neglect your feet, they will make you pay with every literal step you take.
Surgical Treatment
Although most patients with plantar fasciitis respond to non- surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstays of long-term treatment for plantar fasciitis.
Prevention
It is possible to prevent arch pain by wearing well-fitting shoes while performing any physical activity. Many times doctors will suggest a therapeutic shoe with a higher heel to relieve the pressure on the achilles tendon and also the arch muscle (plantar fasciitis). People with arch pain suffer from regular flare-ups of pain. However there is no risk to others as this is not a contagious condition.
Stretching Exercises
Stretching your calf and Achilles tendon may also help as a tight Achilles can make your foot overpronate. To stretch your calf and Achilles tendon, step forwards with your left leg and bend it, with your right leg straight and both feet pointing forwards. Push your right heel into the ground while keeping your right leg straight; you should feel the stretch at the back of your right leg, below the knee. Hold the stretch for 15 to 30 seconds and repeat with the opposite leg. Repeat the stretch two to four times on each leg, and repeat the overall exercise three to four times a day.
Plantar fasciitis is a common and often persistent kind of repetitive strain injury afflicting runners, walkers and hikers, and nearly anyone who stands for a living, cashiers, for instance. It causes mainly foot arch pain and/or heel pain. Morning foot pain is a signature symptom. Plantar fasciitis is not the same thing as heel spurs and flat feet, but they are related and often confused. Most people recover from plantar fasciitis with a little rest, arch support (regular shoe inserts or just comfy shoes), and stretching, but not everyone. Severe cases can stop you in your tracks, undermine your fitness and general health, and drag on for years.

Causes
In most cases, plantar fasciitis develops without a specific, identifiable reason. There are, however, many factors that can make you more prone to the condition. Tighter calf muscles that make it difficult to flex your foot and bring your toes up toward your shin. Obesity. Very high arch. Repetitive impact activity (running/sports). New or increased activity.Although many people with plantar fasciitis have heel spurs, spurs are not the cause of plantar fasciitis pain. One out of 10 people has heel spurs, but only 1 out of 20 people (5%) with heel spurs has foot pain. Because the spur is not the cause of plantar fasciitis, the pain can be treated without removing the spur.
Symptoms
The primary symptom is pain or aching in the arch area. This can be accompanied by inflammation and tenderness. If the pain is caused by the plantar fascia, it is likely to be considerably more severe in the mornings due to the muscles being unused. If you notice that the twinges of pain you have are most commonly associated with or immediately after exercise, you might want to visit a good athletic shoe store to make sure you are wearing the right kind of shoe. Another cause of arch pain is plantar fasciitis. The plantar fascia is a tough tissue structure that holds the bottom part of the arch in place. The fascia often becomes inflamed and sore, usually as a result of repetitive motion (for example, very common in those who stand on their feet for work). The pain is often noticeable first thing in the morning and worse with activity.
Diagnosis
To come to a correct diagnosis, your podiatrist will examine your foot by using his or her fingers to look for a lump or stone bruise in the ball of your foot. He or she will examine your foot to look for deformities such as high or low arches, or to see if you have hammertoes. He or she may use x-rays, MRIs (magnetic resource imaging), and CT scans to rule out fractures and damage to ligaments, tendons, and other surrounding tissues. Your doctor will also inquire about your daily activities, symptoms, medical history, and family history. If you spend a lot of time running or jumping, you may be at a higher risk for pain in the bottom of your foot. These diagnostic tests will help your doctor come to a proper diagnosis and create an appropriate treatment plan.
Non Surgical Treatment
There are many different causes of and treatments for flat foot. The most important part of treatment is determining the exact flat foot type on an individual basis, and doing so early on. The main objective is to become educated on the potential problems, so that you can stop them before they start. Conservative treatment is often successful if initiated early. The old adage "a stitch in time saves nine" definitely applies to the human body, hopefully more figuratively than literally. Do not ignore what your common sense and your body are telling you. Yes, you can live without an arch, but never neglect a symptomatic foot. If you neglect your feet, they will make you pay with every literal step you take.
Surgical Treatment
Although most patients with plantar fasciitis respond to non- surgical treatment, a small percentage of patients may require surgery. If, after several months of non-surgical treatment, you continue to have heel pain, surgery will be considered. Your foot and ankle surgeon will discuss the surgical options with you and determine which approach would be most beneficial. No matter what kind of treatment you undergo for plantar fasciitis, the underlying causes that led to this condition may remain. Therefore, you will need to continue with preventive measures. Wearing supportive shoes, stretching, and using custom orthotic devices are the mainstays of long-term treatment for plantar fasciitis.
Prevention
It is possible to prevent arch pain by wearing well-fitting shoes while performing any physical activity. Many times doctors will suggest a therapeutic shoe with a higher heel to relieve the pressure on the achilles tendon and also the arch muscle (plantar fasciitis). People with arch pain suffer from regular flare-ups of pain. However there is no risk to others as this is not a contagious condition.
Stretching Exercises
Stretching your calf and Achilles tendon may also help as a tight Achilles can make your foot overpronate. To stretch your calf and Achilles tendon, step forwards with your left leg and bend it, with your right leg straight and both feet pointing forwards. Push your right heel into the ground while keeping your right leg straight; you should feel the stretch at the back of your right leg, below the knee. Hold the stretch for 15 to 30 seconds and repeat with the opposite leg. Repeat the stretch two to four times on each leg, and repeat the overall exercise three to four times a day.
Adult Aquired FlatFoot
Overview
Adult acquired flatfoot is normally a complex disorder, together with diverse signs and varying levels of deformity and also disability. There are several forms of flatfoot, almost all associated with which might have one characteristic within common-partial or perhaps total collapse (loss) in the arch. Additional characteristics shared through most types of flatfoot consist of ?Toe drift,? the place where the toes along with front a part of the foot point outward. Your heel tilts toward the outside and the ankle appears to show in. A New brief Achilles tendon or perhaps calf muscle, which usually leads to the heel to lift off the particular ground earlier when strolling and may work as a new deforming force. Within addition, additional deformities such bunions as well as hammertoes could occur and cause pain within people with versatile flatfoot. Well Being problems for example rheumatoid arthritis, diabetes and weight problems can easily boost the particular risk of developing flatfoot and may (or might not) allow it to end up being able to be more difficult to treat. This kind of article provides a short overview of the issues in which can lead to AAFD. Further details concerning probably the actual most typical circumstances that cause an acquired flatfoot in supplement to their remedy options are provided within separate articles. Hyperlinks to people articles are provided.

Causes
A person along with flat feet offers higher load positioned about the posterior tibial tendon that is the main tendon unit supporting up your arch of the foot. All Through life, aging contributes to decreased power of muscles, tendons along with ligaments. Your blood supply diminishes for you to tendons together with aging as arteries narrow. Heavier, obese patients convey more excess weight about the arch and furthermore have higher narrowing of arteries credited to become able to atherosclerosis. In some people, your posterior tibial tendon finally offers out or tears. This is not just a sudden event in many cases. Rather, it is truly a slow, gradual stretching then inflammation along with degeneration in the tendon. As Quickly As the posterior tibial tendon stretches, the actual ligaments with the arch stretch and also tear. the bones in the arch then move out of place along with entire body excess weight pressing down through above. the foot rotates inward in the ankle in a movement known as pronation. The Particular arch appears collapsed, and furthermore the heel bone is actually tilted to the inside. The Actual deformity could progress until the particular foot literally dislocates outward through below the particular ankle joint.
Symptoms
As distinct forms of flatfoot have got different causes, your connected signs can easily be different for various people. Several generalized signs and also symptoms are usually listed. Pain across the length of the particular posterior tibial tendon which in turn lies around the inside of the foot and also ankle. This specific may be connected together with swelling about the inside with the ankle. Pain that's a whole lot worse together with activity. high intensity or impact activities, for example operating along with jumping, can be very difficult. A Few patients could have difficulties walking or perhaps standing for extremely long durations of energy and could even encounter pain with the interior in the ankle and inside the arch of the foot. feeling similar to 1 is ?dragging his or her foot.? When the foot collapses, your heel bone might shift position and put strain on the outside ankle bone (fibula). This may cause pain within the bones and also tendons in the outside regarding the ankle joint. Patients using a vintage injury or arthritis within the core foot may have got painful, bony bumps about the leading along with inside with the foot. These types of create shoe use extremely difficult. Sometimes, the particular bony spurs are generally thus huge which they pinch your nerves which usually can result in numbness and also tingling about the top of your foot and also into the toes. Diabetic patients may well not expertise pain if they've got damage to their nerves. they may possibly recognize swelling or a sizable bump on the bottom with the foot. the huge bump may cause skin problems plus an ulcer (a sore that will not heal) might develop if proper diabetic shoe don just isn't used.
Diagnosis
Clinicians have to recognize your early stage regarding this syndrome which include pain, swelling, tendonitis and disability. the musculoskeletal portion in the clinical exam can help determine happens in the disease. It is really important to palpate the actual posterior tibial tendon as well as test its muscle mass strength. This is tested through asking affected person to plantarflex as well as invert your foot. Joint range of motion is should be assessed as well. Stiffness with the joints may indicate longstanding disease causing any rigid deformity. The weightbearing examination should be performed as well. A New total absence of your medial longitudinal arch is often seen. Throughout later on phases the head with the talus bone projects outward towards the point of a big "lump" within the arch. Observing the patient's feet coming from behind exhibits a substantial valgus rotation with the heel. Via behind, your "too many toes" indicator may be observed as well. This may be when there is abducution in the forefoot inside the transverse plane allowing your toes to be seen from behind. Dysfunction with the posterior tibial tendon may be assessed through asking the actual affected person to become able to stand on his/her toes on the affected foot. In case they might be unable to, this signifies the illness can be inside a heightened stage using the tendon probably totally ruptured.
Non surgical Treatment
Footwear provides a significant role, and patients should be asked to use flat lace-up shoes, or even lace-up boots, that accommodate orthoses. Stage I patients may end up being capable of manage having an off the actual shelf orthosis (such as a possible Orthaheel as well as Formthotics). These People may try a laced canvas ankle brace prior to relocating to some casted orthosis. The Particular different casted, semirigid orthoses offer the medial longitudinal arch of the foot and both contain the heel inside a neutral alignment (stage I) or appropriate your outward bent heel to a neutral alignment (stage II). This approach is actually designed to serve numerous functions: to alleviate strain about the tibialis posterior; to make gait much more efficient by holding your hindfoot fixed; and thirdly, to end up being able to stop progression associated with deformity. Devices available to do this would always be the orthosis of the university involving California Biomechanics Laboratory, an ankle foot orthosis, or a removable boot. Any time this method has been used, a pair of thirds regarding patients get excellent for you to superb results.

Surgical Treatment
In cases where cast immobilization, orthoses and also shoe therapy possess failed, surgery will end up being the next alternative. Your objective associated with surgery along with non-surgical treatment method is usually to eliminate pain, quit progression with the deformity as well as boost mobility of the patient. Opinions vary as to the greatest surgical treatment pertaining to adult acquired flatfoot. Processes generally utilized to right your condition consist of tendon debridement, tendon transfers, osteotomies (cutting and also repositioning regarding bone) and joint fusions. (See surgical correction involving adult acquired flatfoot). Patients together with adult acquired flatfoot tend to be suggested for you to talk about thoroughly the benefits vs. risks of most surgical options. Many treatments have got long-term recovery mandating that the appropriate procedure provide in order to supply the best long-term benefit. most flatfoot surgical methods require 6 in order to twelve weeks of cast immobilization. Joint fusion procedures call for eight weeks involving non-weightbearing around the managed foot - meaning an individual will be about crutches for just two months. The Actual main point here is, Make sure all of your non-surgical choices happen for you to be covered before contemplating surgery. Your Current primary goals using virtually any therapy will be to eliminate pain and enhance mobility. Inside many cases, with the properly designed foot orthosis as well as ankle brace, these goals could be performed with out surgical intervention.
Adult acquired flatfoot is normally a complex disorder, together with diverse signs and varying levels of deformity and also disability. There are several forms of flatfoot, almost all associated with which might have one characteristic within common-partial or perhaps total collapse (loss) in the arch. Additional characteristics shared through most types of flatfoot consist of ?Toe drift,? the place where the toes along with front a part of the foot point outward. Your heel tilts toward the outside and the ankle appears to show in. A New brief Achilles tendon or perhaps calf muscle, which usually leads to the heel to lift off the particular ground earlier when strolling and may work as a new deforming force. Within addition, additional deformities such bunions as well as hammertoes could occur and cause pain within people with versatile flatfoot. Well Being problems for example rheumatoid arthritis, diabetes and weight problems can easily boost the particular risk of developing flatfoot and may (or might not) allow it to end up being able to be more difficult to treat. This kind of article provides a short overview of the issues in which can lead to AAFD. Further details concerning probably the actual most typical circumstances that cause an acquired flatfoot in supplement to their remedy options are provided within separate articles. Hyperlinks to people articles are provided.

Causes
A person along with flat feet offers higher load positioned about the posterior tibial tendon that is the main tendon unit supporting up your arch of the foot. All Through life, aging contributes to decreased power of muscles, tendons along with ligaments. Your blood supply diminishes for you to tendons together with aging as arteries narrow. Heavier, obese patients convey more excess weight about the arch and furthermore have higher narrowing of arteries credited to become able to atherosclerosis. In some people, your posterior tibial tendon finally offers out or tears. This is not just a sudden event in many cases. Rather, it is truly a slow, gradual stretching then inflammation along with degeneration in the tendon. As Quickly As the posterior tibial tendon stretches, the actual ligaments with the arch stretch and also tear. the bones in the arch then move out of place along with entire body excess weight pressing down through above. the foot rotates inward in the ankle in a movement known as pronation. The Particular arch appears collapsed, and furthermore the heel bone is actually tilted to the inside. The Actual deformity could progress until the particular foot literally dislocates outward through below the particular ankle joint.
Symptoms
As distinct forms of flatfoot have got different causes, your connected signs can easily be different for various people. Several generalized signs and also symptoms are usually listed. Pain across the length of the particular posterior tibial tendon which in turn lies around the inside of the foot and also ankle. This specific may be connected together with swelling about the inside with the ankle. Pain that's a whole lot worse together with activity. high intensity or impact activities, for example operating along with jumping, can be very difficult. A Few patients could have difficulties walking or perhaps standing for extremely long durations of energy and could even encounter pain with the interior in the ankle and inside the arch of the foot. feeling similar to 1 is ?dragging his or her foot.? When the foot collapses, your heel bone might shift position and put strain on the outside ankle bone (fibula). This may cause pain within the bones and also tendons in the outside regarding the ankle joint. Patients using a vintage injury or arthritis within the core foot may have got painful, bony bumps about the leading along with inside with the foot. These types of create shoe use extremely difficult. Sometimes, the particular bony spurs are generally thus huge which they pinch your nerves which usually can result in numbness and also tingling about the top of your foot and also into the toes. Diabetic patients may well not expertise pain if they've got damage to their nerves. they may possibly recognize swelling or a sizable bump on the bottom with the foot. the huge bump may cause skin problems plus an ulcer (a sore that will not heal) might develop if proper diabetic shoe don just isn't used.
Diagnosis
Clinicians have to recognize your early stage regarding this syndrome which include pain, swelling, tendonitis and disability. the musculoskeletal portion in the clinical exam can help determine happens in the disease. It is really important to palpate the actual posterior tibial tendon as well as test its muscle mass strength. This is tested through asking affected person to plantarflex as well as invert your foot. Joint range of motion is should be assessed as well. Stiffness with the joints may indicate longstanding disease causing any rigid deformity. The weightbearing examination should be performed as well. A New total absence of your medial longitudinal arch is often seen. Throughout later on phases the head with the talus bone projects outward towards the point of a big "lump" within the arch. Observing the patient's feet coming from behind exhibits a substantial valgus rotation with the heel. Via behind, your "too many toes" indicator may be observed as well. This may be when there is abducution in the forefoot inside the transverse plane allowing your toes to be seen from behind. Dysfunction with the posterior tibial tendon may be assessed through asking the actual affected person to become able to stand on his/her toes on the affected foot. In case they might be unable to, this signifies the illness can be inside a heightened stage using the tendon probably totally ruptured.
Non surgical Treatment
Footwear provides a significant role, and patients should be asked to use flat lace-up shoes, or even lace-up boots, that accommodate orthoses. Stage I patients may end up being capable of manage having an off the actual shelf orthosis (such as a possible Orthaheel as well as Formthotics). These People may try a laced canvas ankle brace prior to relocating to some casted orthosis. The Particular different casted, semirigid orthoses offer the medial longitudinal arch of the foot and both contain the heel inside a neutral alignment (stage I) or appropriate your outward bent heel to a neutral alignment (stage II). This approach is actually designed to serve numerous functions: to alleviate strain about the tibialis posterior; to make gait much more efficient by holding your hindfoot fixed; and thirdly, to end up being able to stop progression associated with deformity. Devices available to do this would always be the orthosis of the university involving California Biomechanics Laboratory, an ankle foot orthosis, or a removable boot. Any time this method has been used, a pair of thirds regarding patients get excellent for you to superb results.

Surgical Treatment
In cases where cast immobilization, orthoses and also shoe therapy possess failed, surgery will end up being the next alternative. Your objective associated with surgery along with non-surgical treatment method is usually to eliminate pain, quit progression with the deformity as well as boost mobility of the patient. Opinions vary as to the greatest surgical treatment pertaining to adult acquired flatfoot. Processes generally utilized to right your condition consist of tendon debridement, tendon transfers, osteotomies (cutting and also repositioning regarding bone) and joint fusions. (See surgical correction involving adult acquired flatfoot). Patients together with adult acquired flatfoot tend to be suggested for you to talk about thoroughly the benefits vs. risks of most surgical options. Many treatments have got long-term recovery mandating that the appropriate procedure provide in order to supply the best long-term benefit. most flatfoot surgical methods require 6 in order to twelve weeks of cast immobilization. Joint fusion procedures call for eight weeks involving non-weightbearing around the managed foot - meaning an individual will be about crutches for just two months. The Actual main point here is, Make sure all of your non-surgical choices happen for you to be covered before contemplating surgery. Your Current primary goals using virtually any therapy will be to eliminate pain and enhance mobility. Inside many cases, with the properly designed foot orthosis as well as ankle brace, these goals could be performed with out surgical intervention.